LH & FSH Hormone Role in PCOS

In polycystic ovary syndrome (PCOS), there is often a disruption in the normal regulation of hormones, including luteinizing hormone (LH) and follicle-stimulating hormone (FSH), which play important roles in the menstrual cycle and ovarian function. The hormonal imbalances in PCOS contribute to the characteristic symptoms and features of the condition. Here’s a closer look at the roles of LH and FSH in PCOS:
Luteinizing Hormone (LH):
LH is a hormone released by the anterior pituitary gland in response to signals from the hypothalamus. It plays a key role in regulating the female reproductive system.
In women with PCOS, there is often an elevated level of LH relative to FSH. This elevated LH-to-FSH ratio is a hallmark of PCOS and is often used as a diagnostic criterion.
The higher LH levels can lead to increased androgen (male hormone) production by the ovarian theca cells. Elevated androgens contribute to many of the symptoms of PCOS, such as acne, hirsutism (excess hair growth), and irregular menstrual cycles.
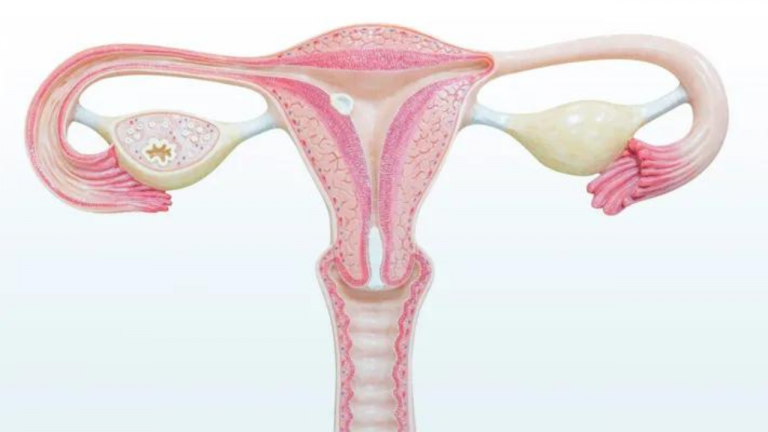
The elevated LH levels can also disrupt normal ovulation. In PCOS, the ovaries may produce multiple small follicles, but these follicles often do not mature properly or release an egg (anovulation). This leads to irregular or absent menstrual periods and fertility issues.
Follicle-Stimulating Hormone (FSH):
FSH is another hormone produced by the anterior pituitary gland, and it is involved in the growth and development of ovarian follicles (structures that contain eggs).
In PCOS, FSH levels may be relatively normal or even lower than LH levels. This imbalance in the LH-to-FSH ratio can contribute to the lack of proper follicle development and ovulation.
Lower FSH levels, in combination with elevated LH levels, can lead to anovulation and the accumulation of small, immature follicles in the ovaries, often referred to as “cysts” (though they are not true cysts).
The hormonal imbalances involving LH and FSH in PCOS are key factors in the development of the syndrome’s characteristic features, including irregular menstrual cycles, anovulation, and the presence of multiple small ovarian follicles. Managing these hormonal imbalances is often a focus of PCOS treatment. Treatment options may include:
Oral Contraceptives: Birth control pills containing estrogen and progestin can help regulate menstrual cycles and reduce elevated androgen levels by suppressing LH.
Anti-Androgen Medications: Medications such as spironolactone or anti-androgenic birth control pills can help reduce androgen-related symptoms like acne and hirsutism.
Ovulation Induction: For women with PCOS who wish to conceive, medications like clomiphene or letrozole can be used to stimulate ovulation.
Lifestyle Modifications: Weight management through diet and exercise can help improve insulin sensitivity and hormonal balance in some cases.
It’s important to note that the specific hormonal profile and response to treatment can vary among individuals with PCOS, so treatment plans should be tailored to each person’s needs and goals. Additionally, PCOS management often involves a multidisciplinary approach that may include consultation with an endocrinologist, gynecologist, or reproductive specialist.